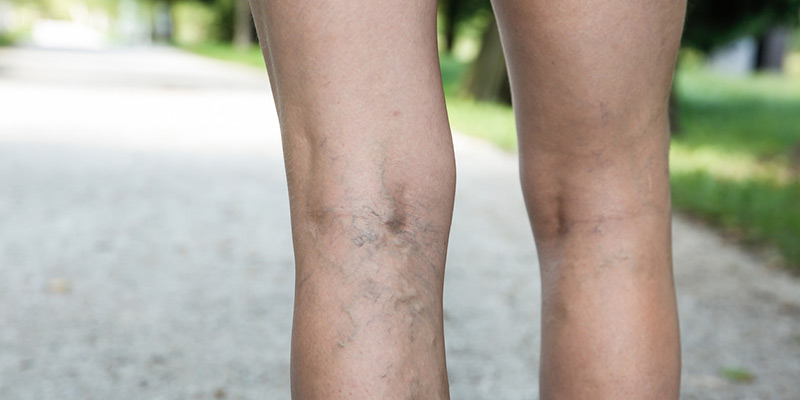
Varicose Veins And What You Can Do About Them
Varicose veins seem like an inevitability for many women. They appear indiscriminately, tracing their scribbled blue lines over once-smooth legs, leaving in their wake a swath of dismay and the desire for answers. So, most importantly, how can they be prevented? What are they? Why do they appear? What are effective treatments? Varicose veins are not insurmountable. Read on to learn preventive measures and how to handle them if they develop.
What Causes Varicose Veins?
We’re all familiar with the sight of varicose veins, like a road map showing the routes blood takes throughout the legs. They can creep up on anyone and, according to the Society for Vascular Surgery, about 35 percent of people in the United States are affected. The tendency to develop varicose veins can be inherited from a parent, but the obese and women who have had multiple children are at higher risk.
Obesity and lack of movement are major contributors to the development of varicose veins, according to the Mayo Clinic. Sitting or standing for long periods of time can negatively impact blood flow. This means that your greatest opportunity to influence your health and appearance in this area is to maintain a healthy weight, exercise routinely and avoid habits of sedentary living.
As the blood in your legs returns to the heart, it’s fighting against gravity. This, according to the Mayo Clinic, is why varicose veins are prominent in the legs. Your veins have valves and flexible walls that aid in the transportation of blood. Age can weaken the elasticity of the veins, allowing the blood that should be moving toward your heart to flow backwards, flooding the veins.
Women are far more likely to develop varicose veins, perhaps in part due to hormonal changes that relax vein walls during pre-menstruation, menopause or pregnancy. Pregnancy also increases the amount of blood in the body, but decreases the blood traveling from the legs to the pelvis, which can contribute to varicose veins.
Are Varicose Veins Dangerous?
Varicose veins, while sometimes unsightly, are not typically dangerous. They may cause pain and discomfort but on their own, they’re typically more of a beauty concern than anything. “In general, varicose veins are a cosmetic problem,” Dr. Elliott M. Antman, a cardiologist, professor of medicine at Brigham and Women’s Hospital at Harvard Medical school in Boston and former president of the American Heart Association said. “Health risks are really related to extremely severe cases.”
In some cases, varicose veins could be an indication of a larger medical problem. Again, the health risks associated with varicose veins are often linked to obesity, lack of movement or cardiovascular problems, according to the American Heart Association. Carrying extra weight around the pelvis, even weight from things like abdominal tumors, could create elevated pressure that can lead to varicose veins. Patients with cardiovascular disease who also have varicose veins, high blood pressure, congestive heart failure or a propensity for water retention, says Dr. Antman, could be more susceptible to swelling in the legs, skin breakdown and infections of the skin that may be a result of varicose veins.
According to the Mayo Clinic, in rare cases varicose veins can cause painful ulcers, especially near the ankles, as a result of long-term fluid buildup from increased blood pressure. Occasionally blood clots can form when legs become swollen or enlarged. This could be a sign of deep vein thrombosis so if you notice this symptom, seek medical attention right away. It’s also imperative that you seek treatment if veins close to the skin burst, causing bleeding.
How Can You Treat Varicose Veins?
Because varicose veins are not often dangerous, most treatments are for comfort or purely cosmetic reasons. Losing weight and maintaining an active lifestyle can slow down the development of varicose veins, which makes them your first line of defense. To manage aches and swelling associated with varicose veins, compression socks and stockings are available. They typically provide 20 to 30 mmHg of compression and can prevent blood from pooling in the legs, according to the Society for Vascular Surgery.
To truly treat the problem and not just manage the symptoms requires more serious intervention. Ablation therapy is one option. It can be accomplished through laser, radiofrequency or mechanical injection. This procedure takes place in the care of a vascular surgeon, in which the patient is numbed and a catheter is inserted into the vein to administer the treatment. It takes about 20 minutes and is generally effective in relieving the pressure and appearance of varicose veins.
Sclerotherapy may be a solution for gnarled veins that aren’t sufficiently straight for the insertion of a catheter as required for ablation therapy. In sclerotherapy, a small needle is advanced through the vein to inject sclerosant, a chemical that causes spasm and triggers the vein to collapse. Blood flow is rerouted through healthy veins. The collapsed vein is not dangerous, and is no longer visible.